Medical VA for Referrals and Administrative Tasks
Referral coordination tends to feel manageable until the volume picks up. One missed fax or an untracked authorization can hold up a patient’s specialist appointment for days. For clinics running lean front desks, that kind of gap rarely stays contained. It ripples into follow-up calls, provider frustration, and patients who fall through the cracks of a process that was never formally owned by anyone.
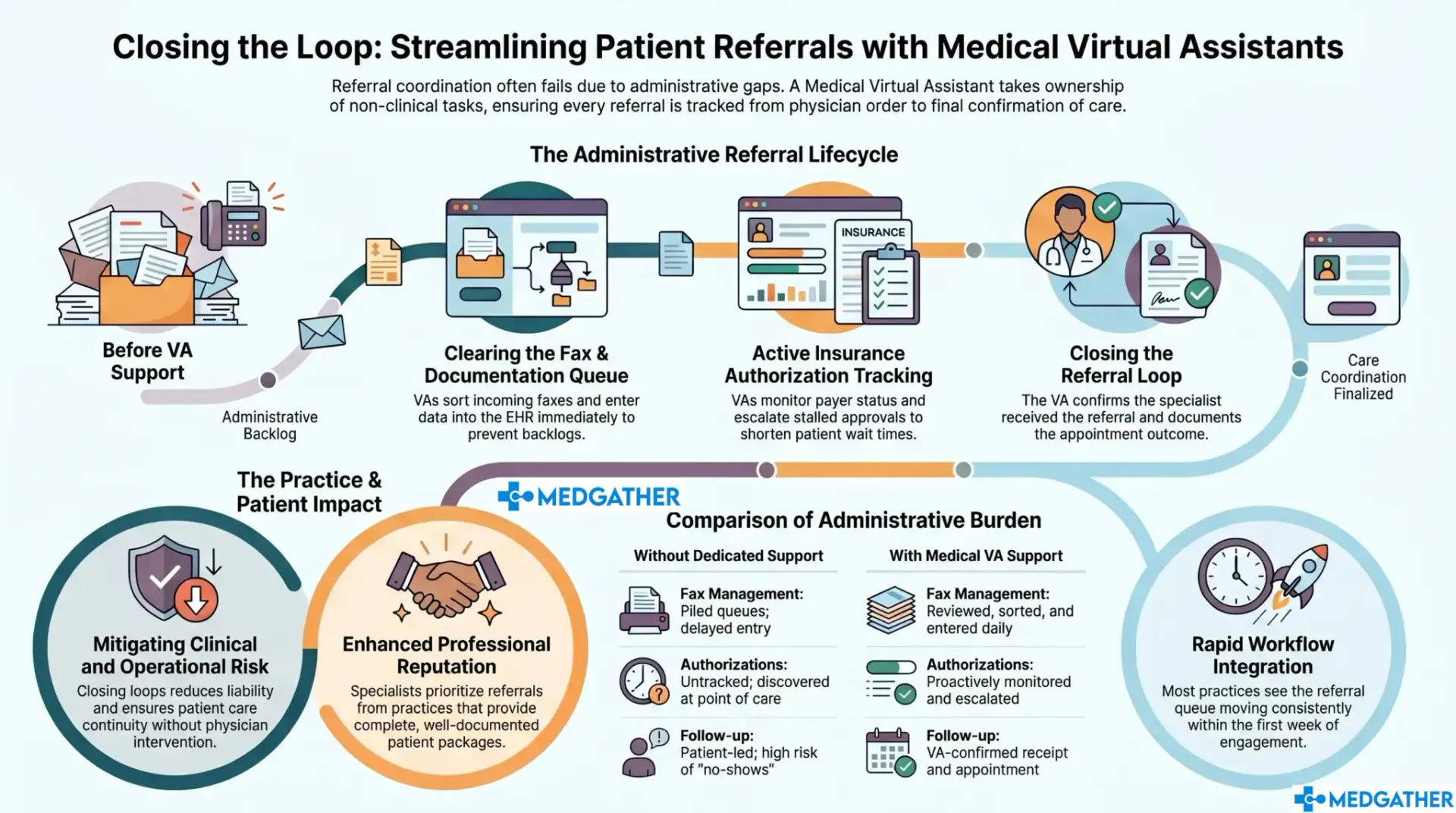
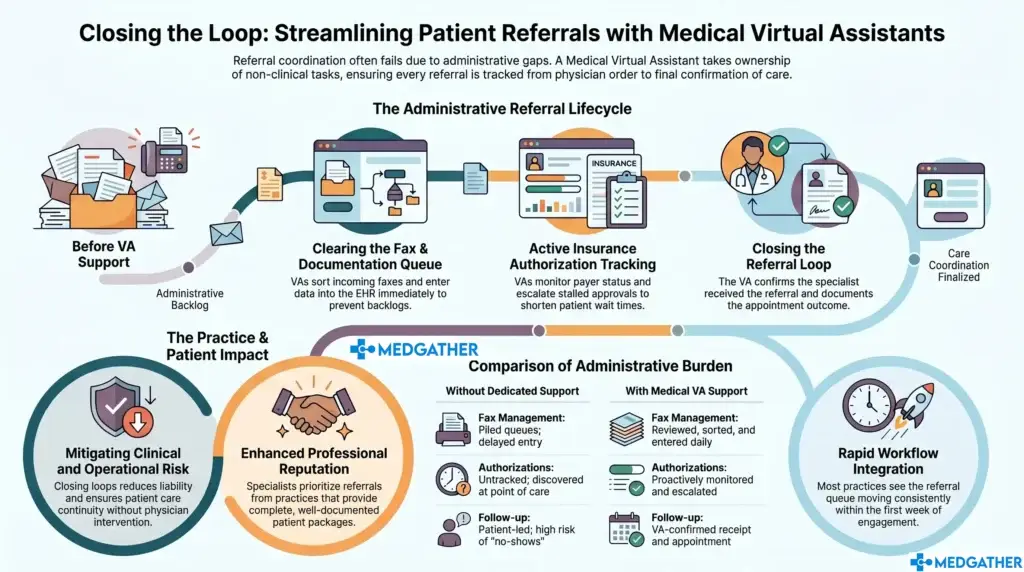
The administrative layer around a referral involves more steps than most clinics account for when staffing the function. The physician makes the clinical decision. The paperwork, the follow-up calls, the insurance authorization tracking, the status checks with the receiving provider, the confirmation that the loop has closed back to the ordering physician, all of that is administrative work. And all of it is where a trained virtual assistant makes the difference.
A medical virtual assistant in a referral support role takes the operational work off the clinical team’s plate, tracking outbound referrals, following up on insurance verification, managing fax queues, making sure documentation is complete before anything moves forward. Here is what that looks like in practice.
What This Support Covers
Referral support at the operational level means the paperwork, the follow-up calls, and the status checks that surround the physician’s clinical decision. The physician makes the referral. The VA makes sure it actually lands, is confirmed by the receiving provider, and is documented accurately before the loop closes.
That final step, confirming the referral was received and acted on, is where most gaps occur. When nobody owns that follow-through, the gap is invisible until a patient calls asking why they have not heard from the specialist. At that point, the practice is already managing the consequences of a breakdown that could have been caught earlier.
Beyond referrals, the same model applies across the broader range of routine administrative tasks. The full list of what a VA handles day to day shows how referral support fits into a broader administrative structure and which functions are typically managed alongside it in a full engagement.
Fax management is one of the functions most directly connected to referral coordination. Incoming referral documents need to be reviewed, sorted, and entered into the EHR correctly before anything downstream can happen. When fax queues pile up, referral processing slows down. When fax management is handled consistently by a dedicated assistant, the queue stays clear and referral documentation moves forward on schedule.
Insurance authorization is the other function where dedicated support has the clearest impact. Waiting on payer approvals is one of the most common sources of referral delays. When someone is actively tracking authorization status, following up when approvals stall, and escalating when timelines are being exceeded, the wait time shortens and the clinical team is not caught off guard when an authorization is denied or delayed at a critical moment.
Why It Matters
Most referral delays come from administrative gaps, not clinical ones. Incomplete documentation and missed follow-ups are far more common causes than anything happening on the clinical side. Left unmanaged, those gaps affect both the clinic’s workflow and the patients waiting on specialist appointments. The impact is not limited to the referral itself. It affects the patient’s confidence in the practice, the ordering physician’s relationship with the receiving provider, and the clinical continuity of the patient’s care.
Keeping the administrative side of referrals consistent prevents small problems from compounding into longer ones. It is also one of the clearest ways a virtual assistant reduces the operational load on clinical staff without requiring any change to how the clinic runs or how the physician practices medicine.
There is a clinical risk dimension to open referral loops that tends to get underweighted in operational conversations. When a referred patient does not receive a follow-up from the specialist and the ordering physician has no confirmation the appointment was kept, the gap creates clinical and operational risk simultaneously. Outcomes can be affected. Liability can be implicated. The administrative function of closing that loop is not just a workflow issue.
For specialty practices where referrals are a primary revenue mechanism, referral coordination quality also directly affects the practice’s reputation with receiving providers. Specialists who receive well-documented, complete referral packages from a practice return calls, prioritize appointments, and build the kind of professional relationship that benefits patients on both ends.
Benefits for Your Practice
When referral support is structured, follow-ups happen on schedule, fax queues stay clear, and documentation issues get caught before they cause delays. For front desks managing multiple providers, dedicated support means fewer things go unattended when the day gets busy. The physician gets confirmation that referrals landed rather than silence.
The benefit to patient experience is also significant. Patients who receive consistent communication about their referral status, who are contacted when there are delays, and who have their specialist appointments confirmed before they show up are patients who feel well cared for. That experience does not happen by accident. It happens when someone owns the follow-through function and executes it consistently.
That kind of consistency changes the day-to-day reality for clinic staff in ways that are hard to see until the backlog is already building. How practices reduce administrative workload without adding headcount covers what that shift looks like operationally once it is in place and what the clinical team typically reports once they are no longer absorbing the referral coordination function.
Common Concerns
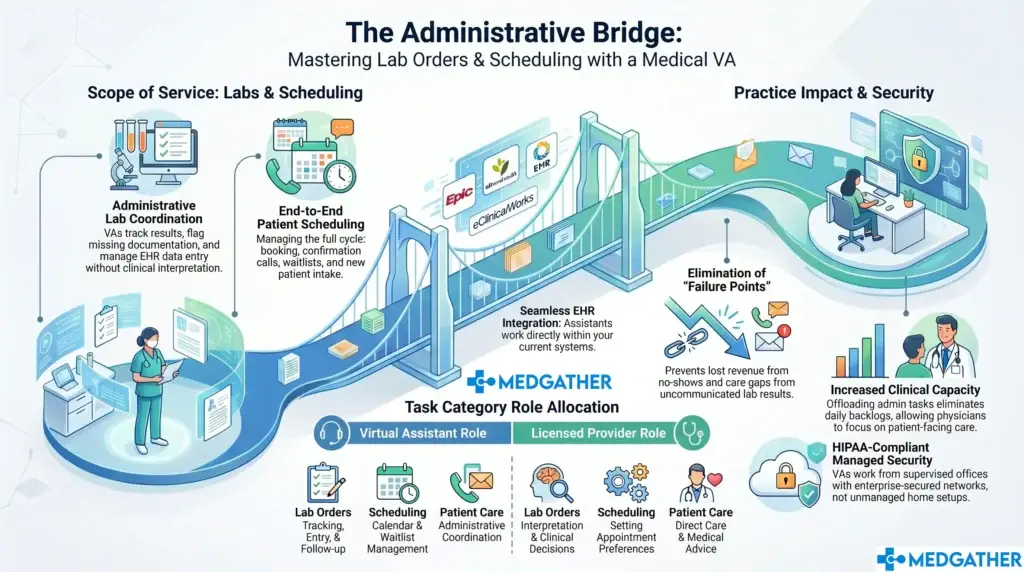
Security is a fair concern when patient information is involved in any remote administrative function. MedGather’s VAs work from a supervised, HIPAA-compliant office environment, and the compliance training they complete covers how patient data is handled at every step of the referral process. The practice retains full control over access and permissions, and nothing moves through the EHR without the clinic’s established documentation protocols being followed.
Accuracy is the other concern that comes up most often around referral coordination. Errors in this function have real consequences: delayed care, insurance complications, documentation gaps that affect billing. MedGather’s low-error standard and supervised team model address this structurally. The oversight is not dependent on the individual assistant’s self-management. It is built into how the team operates every day.
For practices that want more detail on what that security model looks like in practice, why top practices switch to secure virtual medical assistants addresses the most common objections directly and explains what the structural difference between a supervised model and a freelance arrangement means for a clinic handling protected health information daily.
How MedGather Approaches This
Rather than asking a clinic to change how it operates, MedGather fits into the workflow already in place. VAs are briefed on provider preferences, referring relationships, insurance protocols, and practice-specific documentation standards during onboarding. The support they provide is consistent from day one because the briefing is thorough before the assistant handles any tasks.
This approach applies whether the clinic needs referral support alone or a broader administrative arrangement. The onboarding investment is measured in days, not weeks, and the operational improvement is felt within the first week as the referral queue starts moving consistently.
What the full range of remote support looks like for a medical practice, including how each function is managed within a supervised structure, gives a clearer picture of where referral coordination fits and what the assistant is managing alongside it in a typical full engagement.
When referrals are piling up, you should not have to sort through it alone.
Book a free strategy call with MedGather. We will review your current referral workflow and identify exactly where remote support fits -- no commitment required.
Frequently Asked Questions
Can a remote assistant manage fax-based referral workflows?
Yes. Fax review, sorting, and EHR entry are core functions of the referral support role. Incoming referral documents are reviewed, sorted, and entered into the EHR according to the clinic’s process. How this fits into a broader administrative support structure covers the full range of tasks a VA handles alongside referral coordination in a typical engagement.
What happens if a referral has missing documentation?
The VA flags it and follows up according to the clinic’s protocol. Catching those gaps early is where most referral delays get prevented before they become bigger problems. Each VA is briefed on the clinic’s escalation process during onboarding so nothing waits for guidance that should already be in place. If the gap requires clinical input, the appropriate staff member is notified immediately rather than the issue sitting unresolved.
Is this different from what an in-house admin already does?
The tasks are similar but the working structure is not. A remote VA operates within a supervised team rather than as a standalone hire, and that changes how errors get caught and how consistently the work gets done. When a team member leaves, the institutional knowledge of how the referral function works stays within the team rather than walking out the door. How that compares operationally for a clinic is worth reviewing before making a staffing decision.
How quickly can an assistant get up to speed on our referral process?
Onboarding at MedGather is practice-specific. VAs are briefed on workflows, documentation standards, referring relationships, insurance protocols, and provider preferences before handling any tasks. What the hiring and onboarding process looks like walks through the full timeline so there are no surprises on either side. Most practices find the VA is managing the referral function effectively within the first week of full engagement.