What If You Didn't Have to Worry About Paperwork Anymore?
For most healthcare professionals in the United States, the end of the clinical day is not really the end of the workday. The patients are gone, but the documentation, the insurance follow-ups, the inbox are still there. This is not a personal failing. It is a system problem. And it has a solution that more American practices are starting to take seriously: a trained medical virtual assistant who handles the administrative side so the clinical team does not have to
If you want a complete breakdown of how this model works in real-world practice, this medical virtual assistant guide explains the roles, workflows, and benefits in detail.
There is a version of running a medical practice where the administrative side of things runs quietly in the background, handled and organized while you focus on patient care. Appointments coordinated without gaps. Insurance claims followed up before they become problems. Patient communication going out on time, every time. Charts documented correctly and promptly. For a lot of healthcare professionals, that version of their practice sounds like a fantasy. But it is increasingly becoming the operational reality for clinics that have made one structural change: bringing a trained medical virtual assistant into their workflow.
This article is about what that change actually looks like, why it matters more than most practice owners initially expect, and what separates the services that deliver on that promise from the ones that do not.
The Weight That Does Not Show Up on a Schedule
If you ask most healthcare professionals what their biggest challenge is, they will say time. But if you push a little further, what they are really describing is the administrative load. It is the invisible second job that runs parallel to the clinical work and competes with it constantly for attention and energy.
Administrative burnout in healthcare has become one of the most well-documented challenges facing practitioners across the United States. It is not that clinicians are struggling with patient care. They are struggling with everything that surrounds patient care. Chart updates that require an hour of after-hours work. Insurance follow-ups that require a phone call that requires another phone call. Inbox management that starts at 7 AM and somehow never gets to zero.
A landmark study published in the Annals of Internal Medicine found that for every hour physicians spent with patients, they spent nearly two additional hours on administrative tasks and electronic health record documentation, with even more administrative work continuing after hours at home. The study also found that physicians spent more than half of their total working day on desk work and administrative tasks rather than direct patient care.
Source: Sinsky C, et al. “Allocation of Physician Time in Ambulatory Practice.” Annals of Internal Medicine, 2016.
What makes this particularly draining is that the majority of that administrative work does not require clinical expertise. A well-trained medical administrative assistant can handle the vast majority of these tasks, but the systems to make that work efficiently are not always in place, especially in smaller and growing practices. That gap is exactly where a dedicated healthcare virtual assistant steps in.
The issue is not that healthcare professionals lack discipline or efficiency. It is that the administrative work was never designed to be done by the same person doing the clinical work.
This is where the model of a remote medical assistant starts to make practical sense. A trained professional working off-site, within secure systems, handling the operational tasks that pile up every day. Not a temporary fix, but a permanent structural solution. Not a luxury or a workaround, but the right foundation for a practice that is serious about running well.

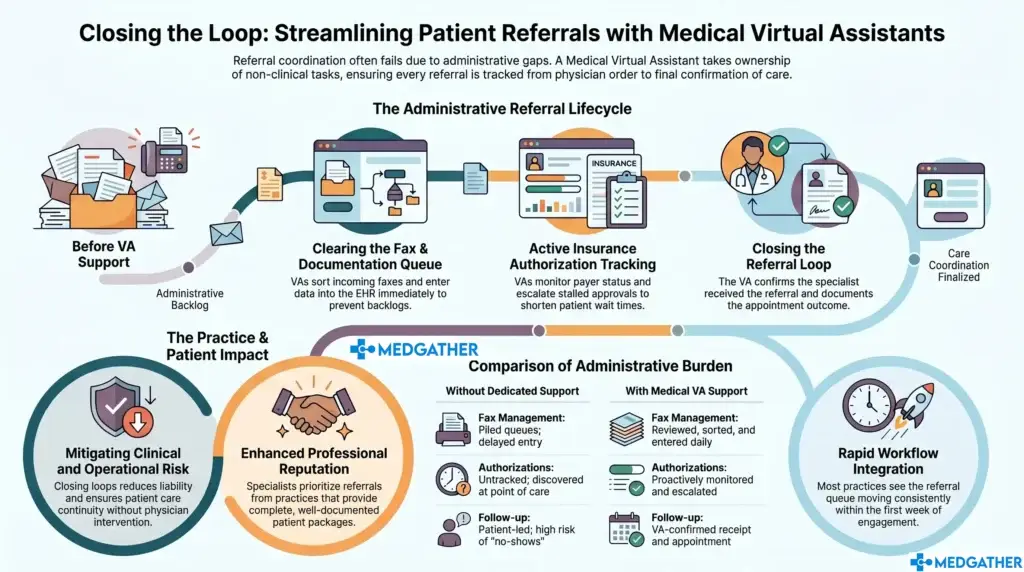
What a Medical Virtual Assistant Actually Does
The term gets used broadly, so it is worth being specific. A medical virtual assistant is not a general-purpose remote worker who happens to be available for healthcare tasks. A properly trained healthcare virtual assistant is someone with specific knowledge of clinical workflows, medical terminology, HIPAA compliance requirements, and the pace of a real practice environment. The distinction matters because the work requires real fluency in how a clinic operates, not just general administrative experience.
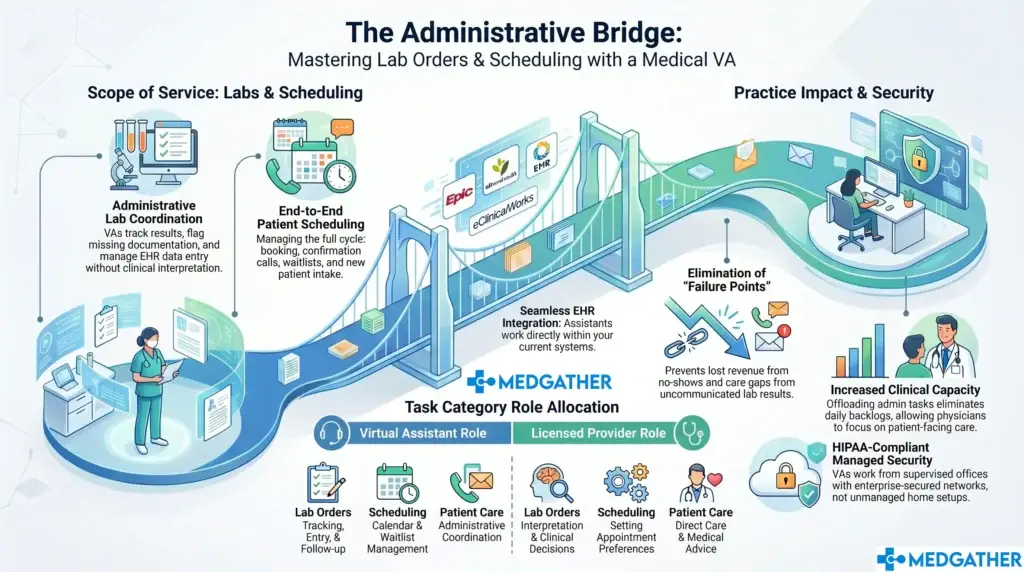
The scope of the work covers the full administrative stack that supports patient care without being part of it. Appointment coordination, including scheduling, rescheduling, confirmations, and calendar management, is one of the most time-sensitive and error-prone areas in any practice. A dedicated VA handles it with the kind of consistency that a busy clinical team often cannot maintain under pressure.
Insurance follow-ups are another core responsibility, and one that directly affects cash flow. Claims that are not followed up on promptly are claims that get delayed or denied. A healthcare virtual assistant who understands insurance workflows and knows how to track, escalate, and resolve outstanding claims is not just saving administrative time. They are protecting revenue.
Patient communication, documentation assistance, and EMR-related administrative tasks round out the typical scope of medical VA services. These are the tasks that tend to stack up at the end of the day when the clinical team is already tired. A remote medical assistant working within a structured system handles them during the day, before they become a problem.
Why the Compliance Question Matters and How It Gets Answered
For any American healthcare professional considering a virtual assistant arrangement, the question of data security and HIPAA compliance is not optional. It is the right question to ask, and the answer needs to be specific.
Working with patient data remotely introduces real risks if the service is not built with the right infrastructure. A general virtual assistant service that has not been designed for healthcare is not an appropriate choice for tasks that involve patient information, regardless of how capable the individual VA might be.
MedGather is built differently. It operates from secure office facilities rather than individual home environments, which provides an additional layer of operational control and accountability that a distributed remote model often cannot match. The systems used to handle patient data are HIPAA compliant and designed specifically for the demands of healthcare administration in the United States. Access controls, data handling protocols, and communication systems are all built around the requirements of US healthcare compliance standards.
This distinction matters because HIPAA compliance is not a checkbox. It is an ongoing operational posture. A service that was designed for healthcare from the ground up handles it differently than one that has adapted general business systems for a clinical context.
The Practical Reality for a Practice That Makes This Change
What actually changes when a US practice brings a trained medical virtual assistant into their workflow? The first thing most practice owners notice is that the end-of-day pile shrinks. The tasks that used to accumulate until someone stayed late to finish them start getting handled during the day, by someone whose full attention is on exactly that work.
The second thing that changes is consistency. One of the most common operational problems in small and growing practices is that administrative tasks get handled differently depending on who is available, what else is happening, and how much pressure the clinical team is under. A dedicated healthcare virtual assistant working within structured processes handles the same tasks the same way every time, which means fewer errors, fewer missed follow-ups, and fewer of the small failures that compound into larger problems over time.
The third change is financial. The cost of hiring medical admin staff locally, when calculated honestly to include training time, benefits, sick leave coverage, and the operational gap every time a position turns over, is significantly higher than most practice owners initially budget for. Choosing to hire a medical virtual assistant through a service like MedGather costs a fraction of an equivalent in-house hire, without the overhead of managing a full-time employee.
For practices that are establishing themselves or actively trying to grow their patient base, that cost difference is not a minor consideration. It is the difference between building administrative infrastructure now versus waiting until the practice is large enough to justify the expense, by which point the lack of structure has already caused real damage.
The Practical Reality for a Practice That Makes This Change
What actually changes when a US practice brings a trained medical virtual assistant into their workflow? The first thing most practice owners notice is that the end-of-day pile shrinks. The tasks that used to accumulate until someone stayed late to finish them start getting handled during the day, by someone whose full attention is on exactly that work.
The second thing that changes is consistency. One of the most common operational problems in small and growing practices is that administrative tasks get handled differently depending on who is available, what else is happening, and how much pressure the clinical team is under. A dedicated healthcare virtual assistant working within structured processes handles the same tasks the same way every time, which means fewer errors, fewer missed follow-ups, and fewer of the small failures that compound into larger problems over time.
The third change is financial. The cost of hiring medical admin staff locally, when calculated honestly to include training time, benefits, sick leave coverage, and the operational gap every time a position turns over, is significantly higher than most practice owners initially budget for. Choosing to hire a medical virtual assistant through a service like MedGather costs a fraction of an equivalent in-house hire, without the overhead of managing a full-time employee.
For practices that are establishing themselves or actively trying to grow their patient base, that cost difference is not a minor consideration. It is the difference between building administrative infrastructure now versus waiting until the practice is large enough to justify the expense, by which point the lack of structure has already caused real damage.

What This Looks Like for Your Practice
The best way to think about a medical virtual assistant is not as a replacement for anything. It is the administrative foundation that should have been there from the beginning. The clinical work is what the practice exists to do. Everything else is support infrastructure. Practices that choose to hire a medical virtual assistant early are not cutting corners. They are building the right structure from the start, with people who specialize in exactly this work.
If your practice is currently absorbing administrative work in ways that are slowing you down, burning out your team, or simply taking time that belongs somewhere else, the question worth asking is not whether a healthcare virtual assistant would help. The question is why you have been carrying the load without one.